
6
VOLUME 14 NUMBER 1 • JULY 2017
REVIEW
SA JOURNAL OF DIABETES & VASCULAR DISEASE
Although there are indications that therapeutic footwear may
be effective in secondary prevention of DFUs,
8
according to some
literature, there are no experimental studies that report on the role
of therapeutic footwear in primary ulcer prevention compared to
normal footwear. This conclusion only came about because one
randomised control trial found no effect of therapeutic footwear
in the secondary prevention of ulcers.
8,20
However other literature
suggests that various designs of therapeutic footwear such as rocker
bottom outsole and half-shoes can effectively off-load at-risk foot
regions, thus preventing ulcer formation or recurrence.
8
Key message:
Therapeutic footwear and custom-made
orthoses are generally used by podiatrists to prevent the
secondary occurrence of DFU.
and MP caused a substantial and additive reduction in pressure (29
to 47%) under the metatarsal heads of the feet by increasing the
contact area of weight-bearing forces when compared to wearing
shoes alone. In addition, it was reported that the MP reduced the
pressure at the metatarsal heads of feet by off-loading the soft
tissue and bone structures proximal to the metatarsal heads.
21
These findings are similar to a study done by Tong and Ng who
investigated the amount of pressure reduction that occurred in feet
when using different types of padding and four insole materials that
are commonly used in podiatry. In this study it was found that all four
commonly used materials, Slow Recovery Poron (SRP), Poron, Poron
+ Plastazote firm (PPF) and Poron + Plastazote soft (PPS), were able
to reduce pressure across the whole foot, with PPF achieving the
most significant result of 28% pressure reduction. The subjects in
this study were also tested with a semi-compressed felt metatarsal
pad (Fig. 3) with an aperture on the first metatarsophalangeal joint
of both feet. The peak pressure in this area showed a significant
reduction of 37% compared to a 29% decrease when PPF was
used alone.
22
Overall, both studies noted that the human foot generally has
increased pressure at the periphery of the aperture site, which,
if not corrected, can cause harmful skin breakdown, and in the
insensate feet of diabetic patients, this can sometimes lead to
severe ulceration. In addition, the pressure responses varied in
the two studies, suggesting that pressure reduction in terms of
using footwear and orthotic devices is highly dependent upon the
condition of the patient’s feet and the patients’ health status, as
well as differences in metatarsal pad material used, including its
size and shape.
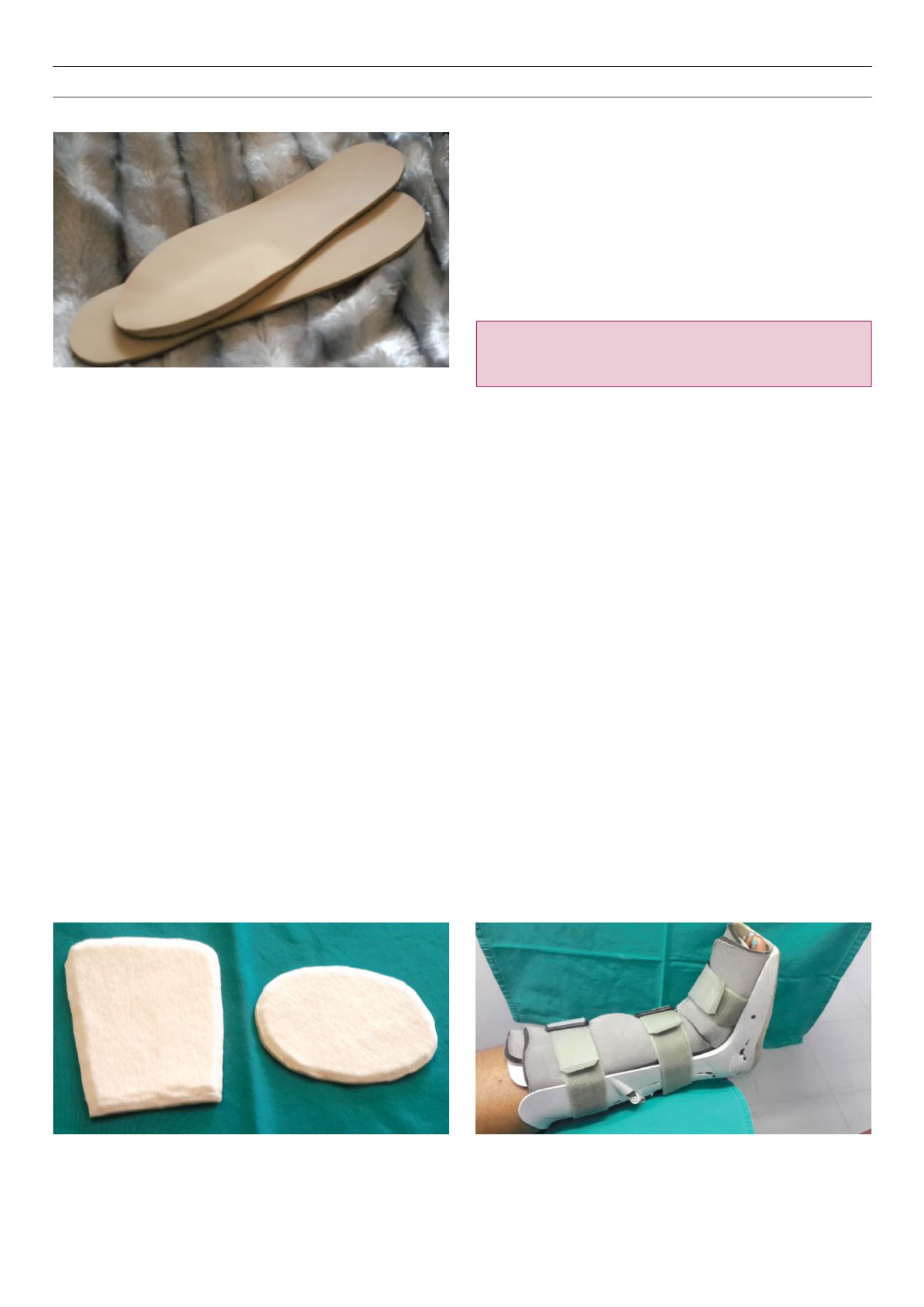
Fig. 2.
Custom-made orthoses.
Fig. 3.
Semi-compressed felt metatarsal pads.
Total-contact casting
Over the years, total-contact casting (TCC) has been known to be
more effective in the treatment of non-infected diabetic plantar
neuropathic ulcers, compared to other removable off-loading
devices. Studies by Sambrook
et al.
noted that TCC has been shown
to reduce plantar pressure by 84 to 94%, and increase healing rates
and treatment time of plantar ulcers.
23
However, TCC is a difficult and time-consuming treatment for
podiatrists to apply and generally there is low patient tolerance, with
a number of side effects associated with its application. Therefore
most clinicians prefer to not use this technique and rather prescribe
various other off-loading techniques that are far easier to apply,
such as felt padding, removable cast walkers (RCW), therapeutic
footwear and orthotic devices.
24
Studies performed by Fife
et al.
using real-world data from a
large wound-care registry found that only 6% of DFU patients
received TCC.
25
Some years later in their reflective analysis, Fife
et
al.
found that in over 25 000 patients with diabetes, only 3.7% of
eligible ulcers received TCC.
26
Currently there are no data on the
use of TCC for the management of DFUs in South Africa.
Alternative approaches of non-removable off-loading devices
that are far more effective have been developed in recent years.
These are a substitute for the classic Plaster-of-Paris total-contact
casting. Armstrong and colleagues performed a study to evaluate
the effectiveness of a RCW (Fig. 4) and an ‘instant’ total-contact
cast (iTCC) (Fig. 5) in the healing of neuropathic DFUs.
27
Patients
with foot ulcers that were cast using iTCC reported more significant
ulcer healing rates of 82.6% over a 12-week period than the 51.9%
healing of patients who received RCW.
Fig. 4.
Removable cast walker.



















