
VOLUME 14 NUMBER 1 • JULY 2017
5
SA JOURNAL OF DIABETES & VASCULAR DISEASE
REVIEW
General DFU management
Management of the diabetic foot often requires a holistic approach,
which involves a focused multidisciplinary team consisting of a
wound nurse, podiatrist, vascular surgeon, endocrinologist and
other allied healthcare professionals.
6,9,13-16
However, the overall
wound management of chronic DFUs can last for extended
periods without any healing response, due to the multiple complex
pathophysiological mechanisms involved in patients suffering from
diabetes. These can involve hypoxia, dysfunction in the fibroblasts
and epidermal cells, impaired angiogenesis and neovascularisation,
high levels of metalloproteases, damage from oxygen radicals
and advanced glycation end-products.
10,17
Peripheral neuropathy
can also contribute to the development and impaired healing of
DFUs. Neuropeptides such as nerve growth factor, substance P and
calcitonin gene-related peptide, and sensory nerves are needed to
induce wound healing, however their low levels in diabetic patients
have been associated with the development of DFUs.
10
Despite all these challenges, there is increasing cause for
optimism in the treatment of diabetic ulcers. This is due to the
enhanced understanding and correction of these pathogenic
factors, combined with stricter adherence to standards of care and
technological breakthroughs in biological agents, and this is giving
new hope to the problem of impaired healing of diabetic ulcers.
18
ulceration but who have foot deformity.
9,19
Different off-loading
techniques are commonly used to protect a diabetic foot from
excessive pressure and other forms of trauma that sometimes lead
to diabetic ulceration or even worse, amputation. These can be
grouped into casting, footwear-related and surgical off-loading
techniques, and other.
20
Off-loading techniques used by podiatrists
in South Africa and overseas include felt padding, prescription
orthotics and insoles, removable cast walkers and total-contact
casting (Figs 2–5).
9,14,15
Key message:
Patients with diabetes mellitus develop foot
problems, such as neuropathy, infections, ulcers and vascular
diseases, which require an integrated multidisciplinary approach
to address all these problems. Failure to adequately treat and
resolve these problems can be due to the multiple complex
pathophysiological mechanisms involved with diabetes, which
is a multisystem disease.
Podiatric DFU management
A podiatrist’s approach to the treatment of DFUs consists of an
overall assessment of the structure and function of the lower limb by
performing biomechanical evaluation, and gait and plantar pressure
analysis. Thus podiatric management and involvement can prevent
diabetic ulcer recurrence in patients through the use of various off-
loading techniques and diabetic patient foot education.
15
Podiatrists also provide patients with local wound care, which
involves debridement of necrotic tissue and callus, cleansing with
suitable solutions, wound dressings, topical or oral antibiotics when
infection is present, and revascularisation.
9,13-15,19
This is the general
standard of wound management that is implemented in diabetic
ulcer wound-care clinics and it involves a multidisciplinary team, as
alluded to earlier.
Key message:
Podiatrists are professionals trained to assess
and implement treatment for diabetic lower limb and foot
problems, including diabetic foot ulcers. Podiatrists manage and
treat diabetic foot through wound debridement, appropriate
wound cleansing and dressings, off-loading, infection control
and education.
Off-loading
Off-loading is an essential tool that is used in the healing of DFUs,
particularly in cases where a patient has a plantar neuropathic
ulcer (Fig. 1), or for secondary prevention in patients with healed
Key message:
Off-loading can be defined as a treatment
modality where practitioners try to protect the foot or reduce
excessive pressure that can lead to ulceration or even amputation
in the diabetic foot. Different off-loading techniques can be
implemented with varying results/success, with some techniques
better than others.
Footwear and orthotic devices for the prevention of DFU
Therapeutic footwear in combination with custom-made orthotic
devices (Fig. 2) are considered the primary means of protecting the
foot from excessive plantar pressure during walking, thus reducing
the incidence of ulceration.
In a study by Mueller
et al.
investigating the effect of total-contact
cast inserts (TCIs) and metatarsal pads (MPs) on metatarsal peak
pressures and pressure–time integrals, it was found that the TCI
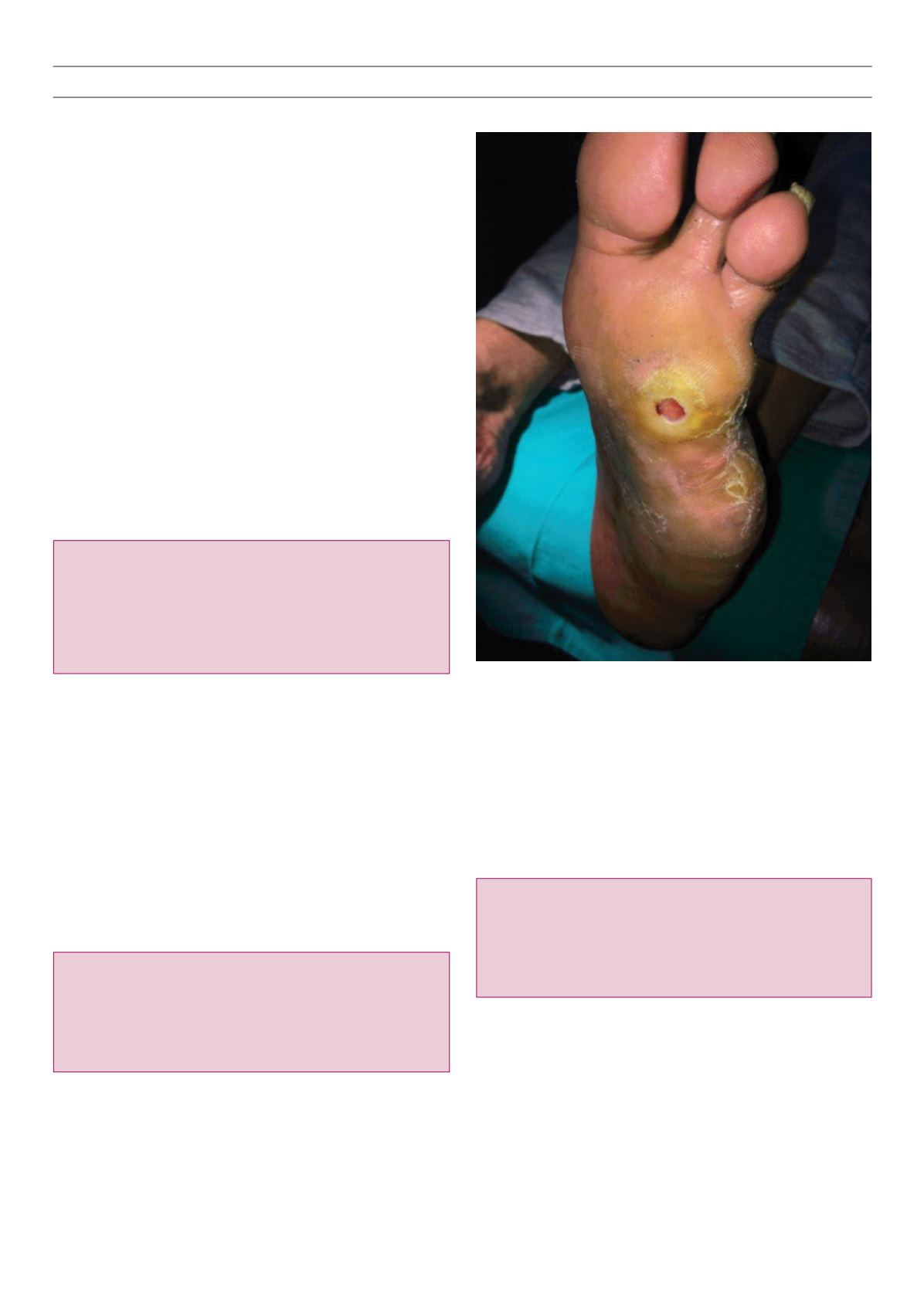
Fig. 1.
Diabetic neuropathic ulcer.



















